Midlife has a way of surprising us.
One minute you’re confidently multitasking like a queen, and the next minute you’re googling: “Why do my knees sound like bubble wrap?”
Welcome to the era where osteoporosis and menopause quietly enter the chat.
The good news? Your bones aren’t broken, you’re not fragile, and this isn’t a doom story. With the right understanding, menopause bone health is something you can actively protect.
Let’s talk bones!
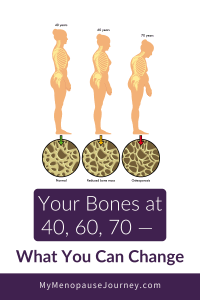

Table of Contents
Osteoporosis and Menopause: What’s the Connection?
Here’s the short version: estrogen is a bone-protecting superstar — and menopause is when estrogen levels drop.
During perimenopause and menopause:
- Bone breakdown speeds up
- Bone rebuilding slows down
- Bone density can decline faster than you realize
In fact, women can lose up to 20% of their bone density in the first five to seven years after menopause. That’s why osteoporosis in midlife is such a big deal — it often begins before you feel anything at all.
Think of it like a silent software update running in the background — except this one’s reshaping your skeleton.
Osteoporosis in Midlife: Why This Stage Matters So Much
Osteoporosis risk doesn’t start to increase in old age — it starts in midlife. This is the window when:
- Bone loss accelerates
- Lifestyle habits make a huge difference
- Prevention works best
The choices you make in your 40s and 50s — movement, nutrition, hormones, sleep — can determine how strong (or brittle) your bones are decades from now.
Midlife isn’t “too late.” It’s actually prime time for bone protection.
The Risk of Osteoporosis: Are You More Vulnerable Than You Think?
Some risk factors you can’t change — but many you can.
Common risk of osteoporosis factors include:
- Hormonal fluctuations in menopause (especially early menopause)
- Family history of fractures or osteoporosis
- Small or thin body frame
- Low calcium — and not enough vitamin D or K2 to help your body actually use it
- Long periods of inactivity
- Smoking or heavy alcohol use
- Chronic stress (yes, cortisol matters)
If you’re thinking, “Cool cool cool, I have three of those” — same, friend. That’s exactly why awareness matters more than panic.
Osteoporosis Symptoms: The Sneaky Ones You Might Miss
Osteoporosis symptoms often don’t show up until a fracture happens. But some subtle signs can include:
- Loss of height over time
- Back pain or stiffness
- Stooped posture
- Fractures from minor falls or movements
If osteoporosis were a person, it would absolutely say, “I’m fine” while quietly rearranging your furniture. This is why screening and prevention — not waiting for symptoms — are key.
Screening: How Do I Even Know If I’m at Risk?
This depends a lot on where you live. In some countries (parts of the US, the UK) postmenopausal women can get a bone density scan — called a DEXA — fairly easily after a certain age or risk profile. In others (much of Europe, Scandinavia, parts of Asia) screening isn’t routine — you only get scanned after you’ve fallen and broken something. Which is, frankly, a backwards way to do prevention.
If you can’t get screened where you live, here’s what I’d think about anyway: Did your mother or grandmother have hip fractures or “shrink” with age? Are you naturally small-framed? Did you go through early menopause? Are you on (or have you been on) long-term steroids, certain anti-seizure meds, or aromatase inhibitors? Have you had a stress fracture or a “weird” break from a minor knock? Any of those put you in higher-risk territory and a private DEXA scan may be worth the cost if you can swing it.
The other useful tool: the FRAX calculator (free online from the University of Sheffield) estimates your 10-year fracture risk from a handful of basic questions. Not a substitute for a scan — but a sensible nudge toward whether to push for one.
DEXA, REMS, QCT, MRI — What’s the Difference?
If you start looking into private scans, you’ll quickly run into a confusing alphabet soup. Quick honest version:
- DEXA (dual-energy X-ray absorptiometry) — the long-standing gold standard. Uses a very low dose of X-ray — about the same as one day of natural background radiation, and less than a single chest X-ray. Quick, accurate, available almost everywhere. The output (your T-score) is what clinical guidelines and the FRAX calculator are built around. If you can only get one scan, this is the one.
- REMS (radiofrequency echographic multi-spectrometry, sold under the brand name Echolight) — the radiation-free ultrasound-based newcomer. Increasingly available at private clinics, including in parts of Europe. Genuine advantages: no radiation at all, portable, can be repeated as often as you like, and isn’t thrown off by spinal arthritis or aortic calcification (which can artificially raise your DEXA score and hide real bone loss). Honest caveat: the evidence is still maturing. A 2026 study in Osteoporosis International raised real questions about how much of the REMS output actually reflects your bone versus the age and weight you typed in. Most physicians still won’t prescribe medication based on REMS alone. Best use right now: as a no-radiation way to track changes over time after one baseline DEXA.
- QCT (quantitative computed tomography) — uses a CT scan to give a 3D measurement of bone density. More sensitive than DEXA at picking up early bone loss in the spine (one study found QCT diagnosed osteoporosis in 46% of postmenopausal women where DEXA only caught 17%). The catch: noticeably more radiation, more expensive, less widely available. Sometimes used when DEXA results don’t match the clinical picture.
- MRI-based bone quality scoring — newest, no radiation, but currently more research than routine. Not something you can just walk in and ask for in most places. One to watch.
The short version: if you’ve never been scanned, start with DEXA — it’s still the reference standard and what every guideline uses. If you want to track yourself yearly without piling up radiation, REMS is reasonable as a follow-up tool — just don’t let anyone tell you it’s straight-up “better” than DEXA. The evidence isn’t there yet.
A Word About Chiropractors and Knocking Backs
I’ll tell you a story on myself. Somewhere around the time I crossed sixty, my back started catching — a sharp twinge, a feeling of weakness I hadn’t had before. I went to a chiropractor who, in the old-school way, did a proper crack of my spine. I felt better for a few days.
My daughter-in-law has since trained as a chiropractor, and she gave me a gentle word: be careful with high-velocity spinal manipulation if you don’t know your bone status. The current research on it is sober — the American College of Rheumatology recommends against forceful spinal manipulation in patients with advanced spinal osteoporosis, and a 2023 review of over a million older adults found that those with osteoporosis who received chiropractic spinal manipulation had a higher risk of fracture. There are published case series of compression fractures in the upper back after adjustments in women whose osteoporosis was undiagnosed at the time.
None of this means “never see a chiropractor.” Many of them work brilliantly with older patients using lower-force, gentler techniques (the Activator method, for example). The point is: tell them your age. Ask about your bone status. Ask what kind of technique they’re planning. And if you don’t know your bone density and you’re past your mid-50s — consider getting that information before letting anyone do anything sudden to your spine.
Menopause Bone Health: What Science Says Actually Helps
Let’s talk solutions — because menopause bone health is not about doing everything perfectly. It’s about doing the right things consistently.
1. Strength Training (and Why Pilates Alone Isn’t Enough)
Bones respond to load. That means:
- Weight training
- Resistance bands
- Bodyweight exercises
No, walking alone isn’t enough (still great for your heart and mind, though). Your bones need a little challenge — like they’re saying, “Oh, we’re still using these? Better stay strong then!”
And here’s a small thing that took me far too long to learn: muscle and bone are not the same project. I spent years doing pilates and lighter strength work, thinking I had the muscle side handled — and I did. But muscle responds to any consistent challenge. Bone needs real load to listen. The kind that makes your bones go, “okay, this is serious, we need to get sturdier.” A 5-pound dumbbell for 20 reps will keep your muscles tidy. It won’t move your bone density.
Research keeps backing this up: postmenopausal women who lift weights consistently — especially with progressive, heavier loads — see meaningful improvements in spine and hip bone density over time. Add a few small jumps or hops where it’s safe to do so, and the loading effect is even stronger. (More on jumping safety further down — it’s not for everyone with established osteoporosis.) Check out the full case for it in strength training for menopause.
Important: take it slow at the start. I cannot say this strongly enough. If you’re new to lifting, get professional help — but please, not a twenty-two-year-old PT whose entire understanding of bones comes from a YouTube short. Find someone (physiotherapist, exercise physiologist, strength coach with a real specialism) who actually understands what osteoporosis means for the body — what to avoid, what positions are risky for the spine, how to progress weight without injuring you, when not to push. The wrong coach with the right intentions can cost you a fracture. The right coach is worth every penny and every hour of finding them.
One tiny add-on I’ve worked into my own routine: on walks, I’ll stop, hop on one leg a handful of times, pause, switch legs, do it again. It sounds silly. It’s based on real research — the British “Hip Hop study” out of Loughborough and the Oregon State weighted-vest work both found single-leg hopping and small daily jumps build hip bone density in postmenopausal women. Costs nothing. Takes thirty seconds. Skip if you have established osteoporosis or knee trouble; check with your doctor first.
While we’re on add-ons: weighted vests have become hugely popular lately, and there’s a real evidence base — even if the hype runs ahead of it. The same Oregon State work I mentioned above used vests during the jumping and resistance exercises (that’s where the <1% vs 3.8% hip bone loss numbers come from). The German EFOPS trial showed similar protective effects.
Dr. Susan Brown, who’s written extensively about natural bone health, makes a point worth hearing: walking alone doesn’t deliver much skeletal load if you’re a thin woman — under 114 lb (52 kg) you’d need over 18,000 steps a day to protect your hips that way, versus around 5,000 for an average-weight woman. A vest helps close that gap. But a 2025 JAMA Network Open trial found that just wearing a vest 8 hours a day during weight loss didn’t prevent hip bone loss — the movement is doing the work, not the vest sitting on you.
Start light (1–2 lb), build up over months not weeks, and skip the vest entirely if you have established spinal osteoporosis or past compression fractures.
2. Calcium + Vitamin D (But Make It Smart)
- Calcium supports bone structure
- Vitamin D helps absorb calcium
- Vitamin K2 helps direct that calcium into your bones (instead of letting it wander off and harden in your arteries — yes, that’s a thing).
- Food first (leafy greens, dairy, sardines), supplements if needed — but avoid megadoses unless your doctor says so.
3. Protein Is Not the Enemy
Because somewhere along the way, protein got blamed for everything from kidney stress to “leaching calcium from bones.”
Thankfully, science has cleared its name.
Here’s the reality: a big chunk of your bone structure — somewhere around 30–50%, depending on how you measure it — is protein, mostly collagen. That protein framework is what gives bones flexibility and strength — without it, bones become brittle, even if you’re getting enough calcium.
Meaning, calcium builds the house, but protein is the scaffolding holding it up.
And for women in midlife, getting adequate protein helps:
- Maintain muscle (which protects bones and balance)
- Improve bone density when combined with strength training
- Reduce the risk of falls and fractures
You don’t need extreme diets or protein shakes at every meal. Just aim for consistent, balanced protein from sources like:
- Eggs, fish, chicken, lean meat
- Greek yogurt, cottage cheese
- Beans, lentils, tofu, tempeh
- Nuts and seeds
A good rule of thumb many experts suggest for midlife women is roughly 30 grams of protein per meal, especially if you’re active or strength training. (More if advised by your healthcare provider.)
Check out my Midlife Protein Calculator to figure out exactly what your number is.
4. Hormones Matter (Yes, We’re Going There)
Estrogen loss is a major driver of osteoporosis and menopause-related bone loss. For some women, menopausal hormone therapy (MHT) can significantly protect bone density when started appropriately.
This is a nuanced decision — personal history matters — and the current Menopause Society guidance puts bone protection firmly back on the list of reasons MHT may make sense, especially when started in early postmenopause.
5. Tools & Tech: What’s New for Midlife Bones
For decades, the bone health conversation was basically: lift things, eat your greens, and maybe take a pill. That’s still the foundation. But the past couple of years have brought some genuinely interesting new tools into the mix — and a few that have been quietly hyped for ages but deserve a closer look.
OsteoBoost: the first FDA-cleared wearable for low bone density. This one’s new enough that most women I talk to haven’t heard of it yet. OsteoBoost is a vibrating belt — worn around the hips for about 30 minutes a day — that delivers gentle, calibrated vibration directly to the hips and lower spine (the two areas most likely to fracture). It got FDA clearance in early 2024 and launched nationwide in May 2025.
The clinical trial behind the clearance (run at the University of Nebraska Medical Center) found postmenopausal women with osteopenia who used it at least three times a week had an 85% reduction in spine bone density loss compared to a sham group. That’s a meaningful number for a non-drug, no-side-effects tool.
It’s prescription-only in the US (you go through your doctor or a telehealth visit), and it’s marketed mostly at women with osteopenia — that’s the in-between zone before full osteoporosis. So it’s not a magic wand and it’s not for everyone. But if you’re sitting with a “low bone density” diagnosis and want something proactive that doesn’t involve bisphosphonates, it’s worth asking your doctor about.
Vibration plates: do they actually do anything? You’ve seen them — the platforms that buzz under your feet while you stand on them. Short answer: there’s real, decent-quality evidence that whole-body vibration platforms can slow bone loss and modestly improve density in postmenopausal women, particularly at the lumbar spine and hip.
One nuance most people miss: it’s not really about your feet and ankles. The vibration enters through your feet, yes — but the goal is for that mechanical signal to travel up through your skeleton to your spine and hips, which is where fractures usually happen. That’s why posture matters so much: standing tall with knees straight (or just very lightly bent) lets the signal travel. Deep squats on a vibration plate look impressive but actually absorb the signal into the leg muscles before it ever reaches your spine.
If you’re considering one: low-magnitude, higher-frequency platforms have the strongest evidence base. Skip the cheap ones that promise weight loss; that’s not what they’re for.
Rebounders (mini-trampolines): the honest version. Rebounders are having a moment, and for good reason — they’re low-impact, joint-friendly, and genuinely fun. My rebounding article walks through the bigger picture.
But here’s the honest take on bones specifically: the evidence is mixed. Some studies show modest spine bone density improvements; others show no significant change. Where rebounders do shine is balance, leg strength, and fall prevention — which matters enormously, because most fractures in midlife and beyond happen because someone fell, not because their bones spontaneously crumbled.
One important caution: if you already have diagnosed osteoporosis (not just osteopenia), check with your doctor before jumping. There are documented cases of compression fractures in the upper back from mini-trampoline jumping in women with established bone loss. Use the rebounder for gentle bouncing and balance work in that case — not high-impact jumps.
OsteoStrong: the once-a-week osteogenic loading studios. You may have a friend who swears by it (I do — my own sister goes every week). OsteoStrong is a franchise of studios where you spend about 10 minutes a week on four specialised machines that let you push against fixed resistance — the idea is to generate brief, very high forces through your skeleton without the joint impact of jumping. It’s marketed heavily at women with osteopenia and osteoporosis, and it has serious franchise presence across the US, UK, Sweden, Australia, and a growing list of countries.
Here’s where it gets honest. The research is real — but it’s also limited and contested.
The big study OsteoStrong points to is a 2025 paper in the Journal of Clinical Endocrinology & Metabolism (a respected journal) on 147 postmenopausal women in Greece. The company’s press release calls it a clean win for bone density. Independent reviewers reading the same data point out that the only groups that showed statistically significant improvement were the ones also taking an osteoporosis medication — OsteoStrong on its own didn’t move the needle on bone mineral density. The study was also a case-series, not a randomised controlled trial, which is a much weaker design.
A separate pilot study from Monash University (Australia) in 2025 followed 44 postmenopausal women with low bone density through 8 months of OsteoStrong. No significant change in hip or spine bone density. Trabecular bone score (a quality measure) actually went slightly down. But — and this matters — chair stand time, stair climb time, and overall physical function clearly improved.
So what’s the takeaway? OsteoStrong probably does what its other branded language hints at: it makes you functionally stronger. Better strength, better balance, faster up out of a chair, more confident on stairs. Those are real fall-prevention wins, and falls are what cause most fractures in midlife. What the independent evidence doesn’t yet support is the big BMD reversal claim. If your sister enjoys it, feels stronger, and it gets her to a weekly appointment she keeps — that’s a genuine win. Just don’t drop your other bone-protective habits assuming the BMD piece is handled.
Bottom line for all four of these tools (OsteoBoost, vibration plates, rebounders, OsteoStrong): they’re not replacements for the basics — lifting heavy-ish things, eating enough protein, getting your calcium-D-K2, and (if appropriate for you) hormone therapy. They’re additions. The basics still do the heaviest lifting, pun fully intended.
Osteoporosis Treatment: What Are the Options?
If bone loss is already happening, osteoporosis treatment isn’t one-size-fits-all.
Options may include:
- Lifestyle and nutrition changes
- Hormone therapy (for eligible women)
- Bone-specific medications that slow breakdown or build bone
- Wearable vibration therapy (like OsteoBoost — covered above)
- Balance work and fall-prevention strategies (underrated but powerful)
The goal isn’t just avoiding fractures — it’s staying mobile, independent, and strong for the long haul.
And the empowering part:
You have more influence over your bone health than most women are led to believe.
Your bones have carried you through everything.
A little support now?
That’s just good reciprocity.
References:
Menopause and bone loss – Cleveland Clinic (health.clevelandclinic.org)
What women need to know about bone loss – Bone Health & Osteoporosis Foundation (bonehealthandosteoporosis.org)
Menopause and bone loss – Endocrine Society (endocrine.org)
The 2022 Hormone Therapy Position Statement – The Menopause Society (menopause.org)
Bone mineral density changes during the menopause transition (SWAN Study) – PMC (pmc.ncbi.nlm.nih.gov)
Demographic determinants of REMS-derived BMD and fragility score – Osteoporosis International (link.springer.com)
Comparison of QCT and DXA: osteoporosis detection rates in postmenopausal women – PMC (pmc.ncbi.nlm.nih.gov)
FRAX fracture risk assessment tool – University of Sheffield (sheffield.ac.uk/FRAX)
Effectiveness of whole-body vibration on bone mineral density in postmenopausal women: meta-analysis – PubMed (pubmed.ncbi.nlm.nih.gov)
Therapeutic effects of whole-body vibration on postmenopausal women with osteoporosis – PMC (pmc.ncbi.nlm.nih.gov)
OsteoBoost FDA De Novo clearance for low bone density – US Food & Drug Administration (fda.gov)
Mini-trampoline jumping as an exercise intervention for postmenopausal women (Fricke et al.) – PMC (pmc.ncbi.nlm.nih.gov)
Mid-thoracic vertebral compression fracture after mini-trampoline exercise: case series – PMC (pmc.ncbi.nlm.nih.gov)
Brief, low-impact, high-intensity osteogenic loading in postmenopausal osteoporosis (Papadopoulou-Marketou et al.) – Journal of Clinical Endocrinology & Metabolism (academic.oup.com/jcem)
Feasibility, safety and efficacy of OsteoStrong in postmenopausal women with low bone mineral density: pilot study – PMC (pmc.ncbi.nlm.nih.gov)
High-intensity hopping exercise to improve hip bone strength in older men: Hip Hop study – NCSEM-EM / Loughborough University (ncsem-em.org.uk)
Long-term exercise using weighted vests prevents hip bone loss in postmenopausal women (Snow et al.) – Journal of Gerontology / Oregon State University (news.oregonstate.edu)
Compression fractures in patients undergoing spinal manipulative therapy – PubMed (pubmed.ncbi.nlm.nih.gov)
Retrospective analysis of severe adverse events from chiropractic spinal manipulation in older adults – PMC (pmc.ncbi.nlm.nih.gov)
Vitamin K2 and bone health – National Center for Complementary and Integrative Health (nccih.nih.gov)
Osteoporosis and menopause – Mayo Clinic (mayoclinic.org)
Long-term exercise using weighted vests prevents hip bone loss in postmenopausal women (Snow et al.) – Journal of Gerontology (academic.oup.com)
Benefits of 2 years of intense exercise on bone density: Erlangen Fitness Osteoporosis Prevention Study (Kemmler et al.) – Archives of Internal Medicine (jamanetwork.com)
Weighted vest use or resistance exercise to offset weight loss–associated bone loss in older adults: randomized clinical trial – JAMA Network Open / PMC (pmc.ncbi.nlm.nih.gov)


Gita is the founder of My Menopause Journey. Since 2014, she has been supporting midlife women by sharing hard-earned learnings from her own experience. To advance her knowledge, Gita puts a lot of her time and effort into understanding the broad spectrum of women’s health. She immerses in extensive research about the physical, mental and emotional aspects of menopause. Gita believes in the life-changing power of healthy, holistic living — this is where she anchors her message to all women. Learn more about her marvelous mission in About us - My Menopause Journey.





most of the people go for various ways to cure this..but after reading this helpful information i would suggest to people to go for this Ayurvedic treatment..no side effect for sure..Thanks for sharing
Hi Amit,
Thanks for sharing your experience about Ayurveda. Come back anytime!
Have a great day!
Gita